Sensory testing of the glossopharyngeal nerve is an important diagnostic procedure that can provide valuable insights into the functioning of this vital cranial nerve. The glossopharyngeal nerve, also known as the ninth cranial nerve (CN IX), is responsible for several crucial functions, including taste sensation in the posterior one-third of the tongue, monitoring blood pressure, and sensory innervation of the pharynx and carotid sinus. In this article, we will discuss the anatomy and functions of the glossopharyngeal nerve, the necessary equipment for the sensory test, patient preparation guidelines, the step-by-step procedure for conducting the test, interpreting the test results, potential complications and risks, as well as post-test care and follow-up.
Understanding the Glossopharyngeal Nerve
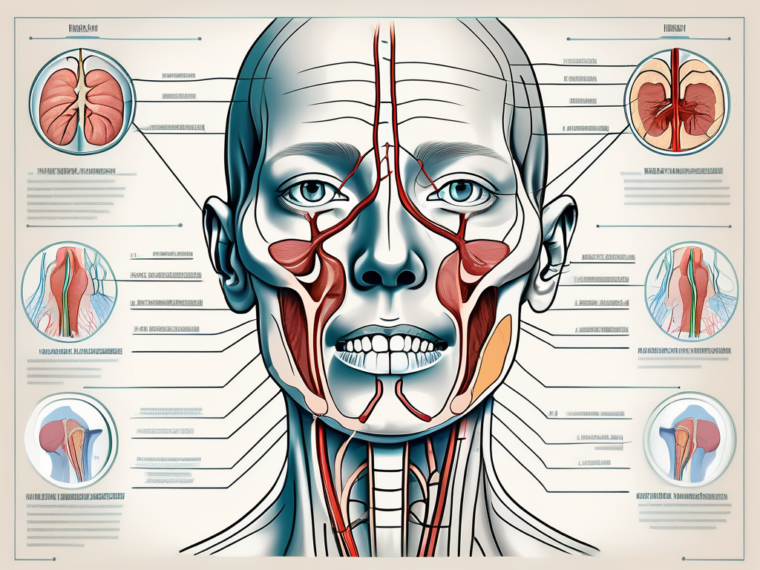
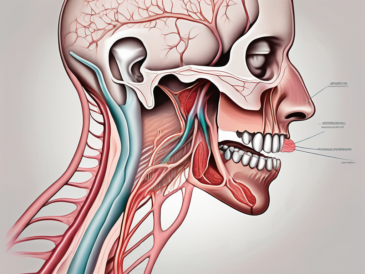
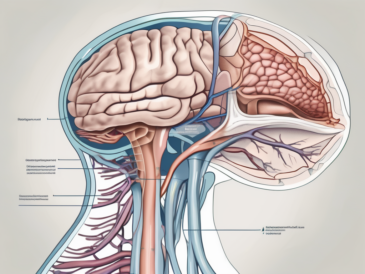
The glossopharyngeal nerve plays a crucial role in various sensory and motor functions within the head and neck region. It is one of the twelve cranial nerves that originate directly from the brain and exit the skull through designated foramina. The course of the glossopharyngeal nerve begins at the brainstem and extends downward into the jugular foramen, where it travels alongside other important nerves and blood vessels.
The glossopharyngeal nerve is a fascinating component of the human nervous system. Its intricate anatomy and multifaceted functions contribute to the overall well-being and functionality of individuals. Let’s explore the anatomy and functions of this remarkable nerve in more detail.
Anatomy of the Glossopharyngeal Nerve
Before delving into the sensory testing procedure, it is important to understand the anatomical course of the glossopharyngeal nerve. The nerve originates from the medulla oblongata, specifically from the posterior aspect of the brainstem. It emerges from the skull through the jugular foramen and extends downwards, giving off branches that supply various structures in the head and neck region.
The glossopharyngeal nerve has multiple branches, each with its own unique role. One of these branches is the tympanic nerve, which provides sensory innervation to the middle ear. This allows for the perception of sound and helps maintain equilibrium. Another branch is the lingual nerve, which conveys taste sensation from the posterior one-third of the tongue. This enables individuals to experience the diverse flavors of the foods they consume.
Additionally, the glossopharyngeal nerve also carries parasympathetic fibers that contribute to the regulation of salivation and assist in the control of blood pressure. These intricate connections within the nerve network highlight its importance in maintaining overall physiological balance.
Functions of the Glossopharyngeal Nerve
The glossopharyngeal nerve serves several important functions that are crucial for proper functioning of the oral and pharyngeal regions. As previously mentioned, one of its primary functions is taste sensation, specifically in the posterior one-third of the tongue. This allows individuals to appreciate different flavors and enhances the overall enjoyment of food and beverages.
In addition to taste sensation, the glossopharyngeal nerve also contributes to the regulation of blood pressure. It contains specialized baroreceptor cells located in the carotid sinus, which monitor changes in blood pressure and relay this information to the brain. This feedback loop helps maintain blood pressure within a normal range and ensures adequate perfusion of organs and tissues.
Furthermore, the glossopharyngeal nerve plays a vital role in the coordination of swallowing and speech. It provides sensory innervation to the pharyngeal muscles, allowing for the detection of food bolus movement and triggering the appropriate motor response. This intricate coordination ensures efficient swallowing and clear articulation during speech.
Understanding the intricate functions of the glossopharyngeal nerve provides insight into the complexity of the human nervous system. Its role in taste sensation, blood pressure regulation, and coordination of swallowing and speech highlights its importance in maintaining overall health and well-being.
Preparing for the Sensory Test
When it comes to conducting a sensory test of the glossopharyngeal nerve, proper preparation is key. Not only does it ensure accurate results, but it also guarantees the safety and comfort of the patient. Let’s take a closer look at the necessary equipment and patient preparation guidelines.
Necessary Equipment for the Test
Before diving into the sensory test, it is crucial to have all the necessary equipment readily available. This typically includes a sterile cotton swab, a tongue depressor, a standard light source, and gloves. These items are essential not only to ensure proper hygiene but also to prevent the risk of infection.
Let’s start with the sterile cotton swab. This tool is used to gently stimulate the glossopharyngeal nerve, allowing for the assessment of sensory function. By using a sterile swab, we minimize the risk of introducing any foreign substances that could potentially interfere with the results.
Next, we have the tongue depressor. This instrument helps to keep the tongue in place during the test, making it easier to access the glossopharyngeal nerve. It also aids in preventing the patient from accidentally biting down on the swab, ensuring their safety throughout the procedure.
A standard light source is another essential piece of equipment. It provides adequate illumination, allowing the examiner to clearly visualize the area being tested. This is crucial for accurate assessment and ensures that no details are missed during the examination.
Lastly, gloves are a must-have. Not only do they protect the examiner from potential pathogens, but they also maintain a sterile environment, reducing the risk of contamination. Wearing gloves is an essential part of maintaining proper hygiene throughout the sensory test.
Patient Preparation Guidelines
Proper patient preparation is crucial for the accurate and safe conduct of the sensory test. It is not just about having the right equipment; it also involves creating a comfortable and supportive environment for the patient. Let’s delve into the guidelines for patient preparation.
First and foremost, it is essential to explain the procedure to the patient in detail. This helps to alleviate any concerns or anxieties they may have and ensures that they fully understand what will happen during the test. Clear communication is key to building trust and cooperation with the patient.
Informed consent is another crucial aspect of patient preparation. Before proceeding with the sensory test, the patient must provide their consent after being informed of the potential risks and benefits. This ensures that the patient is fully aware of what they are agreeing to and allows them to make an informed decision about their participation.
Reviewing the patient’s medical history is also an important step. This helps to identify any contraindications or potential risks that may affect the test’s accuracy or the patient’s safety. By understanding the patient’s medical background, the examiner can tailor the sensory test accordingly and take any necessary precautions.
Creating a calm and comfortable environment is crucial for minimizing stress and anxiety during the test. This can be achieved by ensuring a quiet and private space, free from distractions. Additionally, providing emotional support and reassurance to the patient can go a long way in helping them feel at ease.
By following these patient preparation guidelines, we can ensure that the sensory test is conducted accurately and safely, providing valuable insights into the function of the glossopharyngeal nerve.
Conducting the Sensory Test
The sensory test of the glossopharyngeal nerve involves assessing taste sensation in the posterior one-third of the tongue. This test is crucial in evaluating the functionality of the nerve and identifying any abnormalities. By following a step-by-step procedure and taking necessary safety measures, healthcare professionals can accurately perform the test and gather valuable information about the patient’s taste perception.
Step-by-Step Procedure
The following step-by-step procedure outlines how to perform the test:
- Ensure the patient is in a comfortable seated position with good lighting. This will create an optimal environment for the test and help the patient feel at ease.
- Wash hands thoroughly and put on gloves. Hand hygiene is of utmost importance to prevent the spread of germs and maintain a sterile environment.
- Gently depress the tongue using a tongue depressor to provide better visualization of the posterior one-third of the tongue. This step is crucial in ensuring clear visibility and accessibility to the taste buds.
- Moisten a sterile cotton swab with a taste solution, such as a diluted flavored solution, and gently touch it to the posterior one-third of the patient’s tongue. The taste solution should be carefully chosen to provide a variety of flavors for accurate assessment.
- Ask the patient to identify the taste sensation experienced and provide feedback. It is important to encourage the patient to express their perception of taste clearly and honestly.
- Repeat the process with different taste solutions to assess the patient’s ability to distinguish various flavors. By using a range of taste solutions, healthcare professionals can evaluate the patient’s taste discrimination skills.
- Record the patient’s responses and any abnormal findings for further analysis. Accurate documentation of the patient’s taste perception and any deviations from the norm will aid in diagnosis and treatment planning.
Safety Measures During the Test
During the sensory test, it is important to prioritize patient safety and comfort. The following safety measures should be taken:
- Ensure that the tongue depressor is used carefully to avoid unnecessary discomfort or injury. Gentle pressure should be applied to depress the tongue without causing any pain or trauma.
- Use sterile equipment to minimize the risk of infection. Sterile cotton swabs and tongue depressors should be used for each patient to maintain a hygienic testing environment.
- Practice proper hand hygiene by washing hands thoroughly and wearing gloves. This will prevent the transmission of pathogens and maintain a sterile field.
By following these safety measures, healthcare professionals can ensure the well-being of their patients and obtain accurate results during the sensory test of the glossopharyngeal nerve.
Interpreting the Test Results
The interpretation of the sensory test results depends on the patient’s ability to correctly identify taste sensations. Typically, individuals with intact glossopharyngeal nerve function will be able to distinguish different taste sensations accurately. Normal findings indicate that the glossopharyngeal nerve is functioning properly, allowing for appropriate taste perception in the posterior one-third of the tongue. However, abnormal findings may suggest a dysfunction or impairment of the glossopharyngeal nerve, which would require further investigation and evaluation.
When analyzing the results of a sensory test, it is important to consider various factors that may influence taste perception. These factors can include age, gender, smoking habits, medication use, and underlying medical conditions. For example, certain medications can alter taste perception, leading to false abnormal results. Therefore, it is essential to take a comprehensive approach when interpreting the test findings.
Furthermore, it is important to note that taste perception is not solely dependent on the glossopharyngeal nerve. Other cranial nerves, such as the facial nerve and the trigeminal nerve, also play a role in taste sensation. Therefore, if abnormal results are obtained, it is crucial to consider the possibility of involvement of other cranial nerves or even central nervous system disorders.
Implications of Abnormal Results
If abnormal results are obtained during the sensory test, it is important to consider potential underlying causes and associated clinical implications. Abnormal findings may indicate various conditions that can affect the glossopharyngeal nerve, such as nerve damage, infections, or underlying systemic diseases. In such cases, it is crucial to consult with a medical professional for further evaluation and appropriate management.
One possible cause of abnormal sensory test results is glossopharyngeal neuralgia, a condition characterized by recurring episodes of severe pain in the throat, tongue, and ear. This condition can result from irritation or compression of the glossopharyngeal nerve, leading to altered taste perception. Treatment options for glossopharyngeal neuralgia may include medication, nerve blocks, or in severe cases, surgical interventions.
Infections, such as viral or bacterial pharyngitis, can also affect the glossopharyngeal nerve and lead to abnormal sensory test results. These infections can cause inflammation and damage to the nerve, resulting in altered taste perception. Prompt diagnosis and appropriate treatment of the underlying infection are essential for resolving the abnormal findings and restoring normal taste function.
Additionally, certain systemic diseases, such as diabetes or autoimmune disorders, can impact the function of the glossopharyngeal nerve and lead to abnormal sensory test results. In these cases, managing the underlying systemic condition is crucial for improving taste perception and overall oral health.
It is important to remember that abnormal sensory test results do not necessarily indicate a serious or life-threatening condition. However, they should not be ignored, as they may provide valuable insights into the patient’s overall health and help guide further diagnostic investigations.
Potential Complications and Risks
When it comes to the sensory test of the glossopharyngeal nerve, it is generally considered safe and low-risk. However, as with any medical procedure, there are potential complications that may arise, although they are relatively rare. It is important to be aware of these risks and take appropriate precautions to minimize them.
Risks Associated with the Test
During the sensory test, some patients may experience discomfort. This can range from a mild sensation to more significant pain. It is crucial for healthcare professionals to communicate with patients throughout the procedure, ensuring their comfort and addressing any concerns they may have.
In rare cases, minor mucosal trauma may occur during the test. This can happen when the instruments used to stimulate the glossopharyngeal nerve come into contact with the delicate tissues of the throat. Healthcare professionals must exercise caution and use gentle handling techniques to minimize the risk of injury.
Another potential risk is an allergic reaction to the taste solutions used during the test. These solutions are designed to stimulate the glossopharyngeal nerve and assess its sensory function. However, some individuals may have allergies or sensitivities to certain substances. It is essential to screen patients for any known allergies or contraindications before proceeding with the test.
To mitigate these risks, healthcare professionals should follow strict protocols and guidelines. This includes using sterile equipment to minimize the risk of infection and ensuring proper hygiene practices. Additionally, assessing patients for any allergies or contraindications beforehand can help prevent adverse reactions.
Managing Potential Complications
In the event that complications do arise during or after the sensory test, it is crucial to manage them promptly and appropriately. This will help ensure the well-being and comfort of the patient.
If a patient experiences minor discomfort or mucosal trauma, providing symptomatic relief is important. This may involve recommending over-the-counter pain relievers or soothing remedies to alleviate any pain or irritation. Additionally, healthcare professionals should educate patients on proper wound care techniques to promote healing and prevent infection.
In the case of an allergic reaction, immediate action is necessary. Healthcare professionals should be prepared to administer appropriate treatments, such as antihistamines or epinephrine, depending on the severity of the reaction. Patients should also be advised to seek medical attention if their symptoms persist or worsen after the test.
Overall, while the sensory test of the glossopharyngeal nerve is generally safe, it is essential to be aware of the potential complications and risks. By taking appropriate precautions, using sterile equipment, practicing gentle handling techniques, and assessing for allergies or contraindications, healthcare professionals can minimize these risks and ensure the well-being of their patients.
Post-Test Care and Follow-up
Immediate Post-Test Care
After completing the sensory test, it is important to provide appropriate care and support to the patient. This includes ensuring the removal of any taste solutions from the mouth, providing oral hygiene instructions if necessary, and addressing any immediate concerns or questions the patient may have.
Scheduling and Preparing for Follow-up Appointments
Depending on the test results and individual patient circumstances, follow-up appointments may be necessary to further explore any abnormalities or monitor progress. It is recommended that patients consult with a healthcare professional to discuss the next steps, arrange the required follow-up appointments, and obtain appropriate guidance regarding the management of any underlying conditions that may be contributing to abnormal test results.
In conclusion, the sensory testing of the glossopharyngeal nerve is a valuable diagnostic procedure that provides important insights into its functioning. By understanding the anatomy and functions of the glossopharyngeal nerve, assembling the necessary equipment, following proper patient preparation guidelines, and conducting the sensory test with care, accurate and valuable results can be obtained. Interpreting the test results and recognizing potential complications or abnormal findings allows for appropriate follow-up care and management. Consulting with a medical professional is essential to ensure accurate diagnosis, proper management, and optimal patient outcomes.